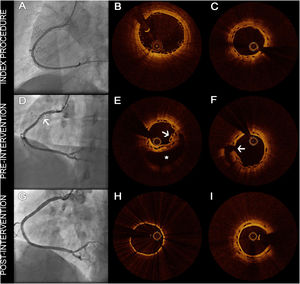
We report the case of a 38-year-old woman with a complicated spontaneous coronary artery dissection (SCAD) of the right coronary artery treated with sequential bioresorbable vascular scaffolds (BVS) making a ‘full plastic jacket’.1 A good angiographic result was achieved (Figure 1A and B). Optical coherence tomography (OCT) showed slight persistence of the proximal dissection (Figure 1C) that was considered non-significant. At one-year follow-up, the patient was admitted for unstable angina. Angiography showed a contrast-filled perivascular space in the proximal segment (Figure 1D, arrow). On OCT, BVS struts were fractured and prolapsing into the lumen (Figure 1E, arrow) and there was a large false lumen with persistent entry flaps (Figure 1E and F, asterisk, arrow). In order to seal the chronic dissection and deal with the fractured BVS struts, a covered coronary stent was implanted. There was angiographic and OCT success (Figure G and H) without BVS damage at the covered stent margins. After six months, follow-up angiography and OCT imaging confirmed a good result of the intervention (Figure 1I).
(A) Index right coronary angiography after angioplasty; (B) index optical coherence tomography (OCT) imaging after angioplasty; (C) index OCT imaging with residual proximal dissection covered by stent struts; (D) suspicious lesion, suggestive of a residual dissection/false aneurysm (arrow); (E) proximal BVS stents with a large hematoma (asterisk), overlapped struts and struts protruding into the lumen (arrow); (F) entry flaps of the residual proximal dissection (arrow); (G) final angiographic result after angioplasty; (H) final OCT showing correct stent expansion and sealing of the flaps; (I) six-month follow-up OCT with no signs of stent restenosis.
Although initial enthusiasm for BVS has waned after results of more recent clinical trials, complicated SCAD is considered a good indication for their use. This case demonstrates that even in this setting there may be non-acute complications that may not be apparent in a non-invasive clinical follow-up. Based on our findings we suggest a low threshold for angiographic and intravascular imaging assessment. Finally, the use of a covered stent in a case of BVS fracture and chronic dissection was safe and effective.
Conflicts of interestThe authors have no conflicts of interest to declare.