A 74-year-old woman with hypertension and dyslipidemia was referred to the cardiology outpatient clinic with dyspnea on moderate exertion. Physical examination was unremarkable. ECG had left ventricular hypertrophy voltage criteria. Transthoracic echocardiogram showed mild dilation of the left chambers and hypokinesia of inferior, posterior and lateral walls with mild depression of left ventricular systolic function. Because of the findings in the echocardiogram she was referred for invasive coronary angiography (CA) without an ischemia test.
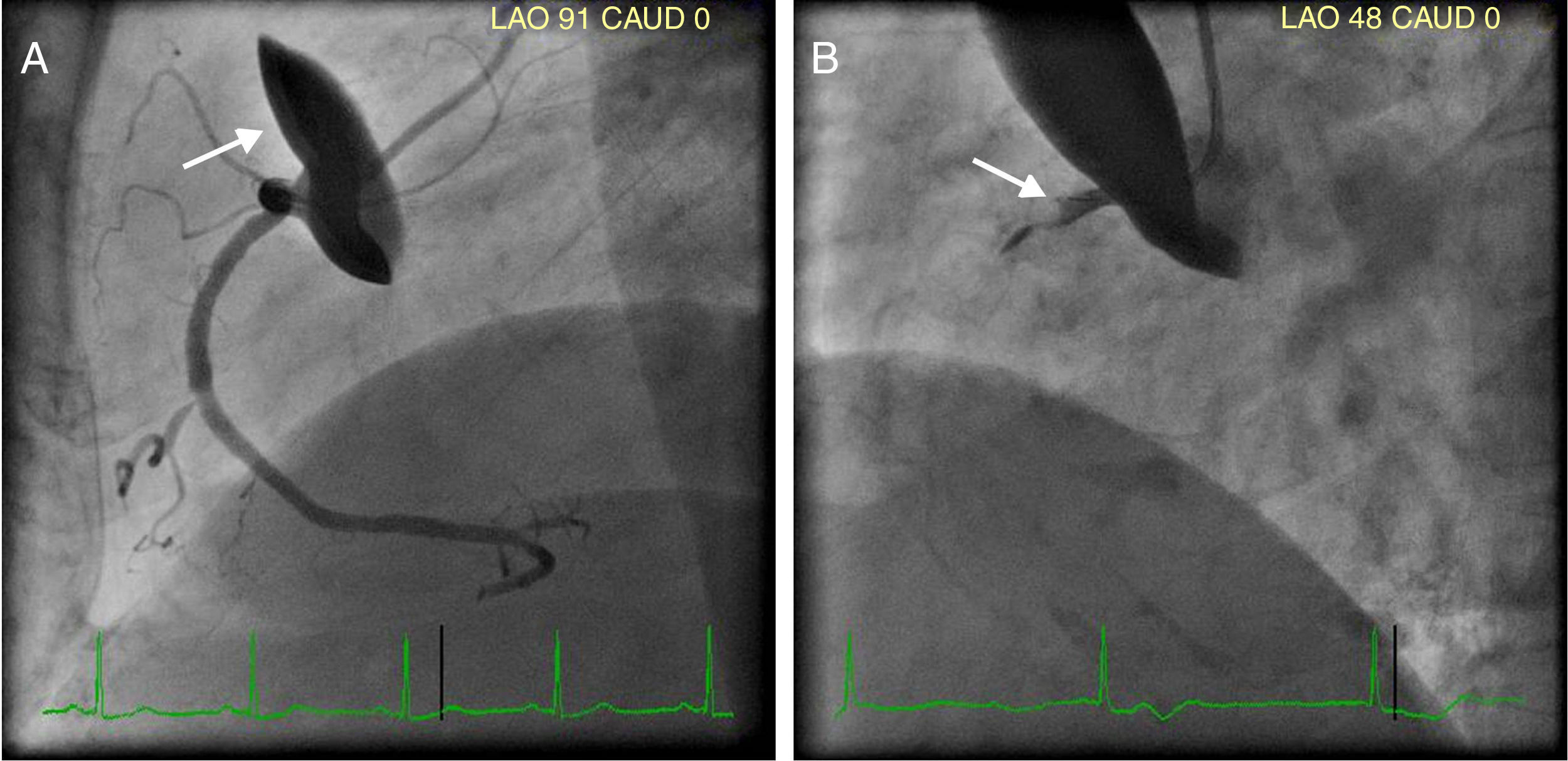
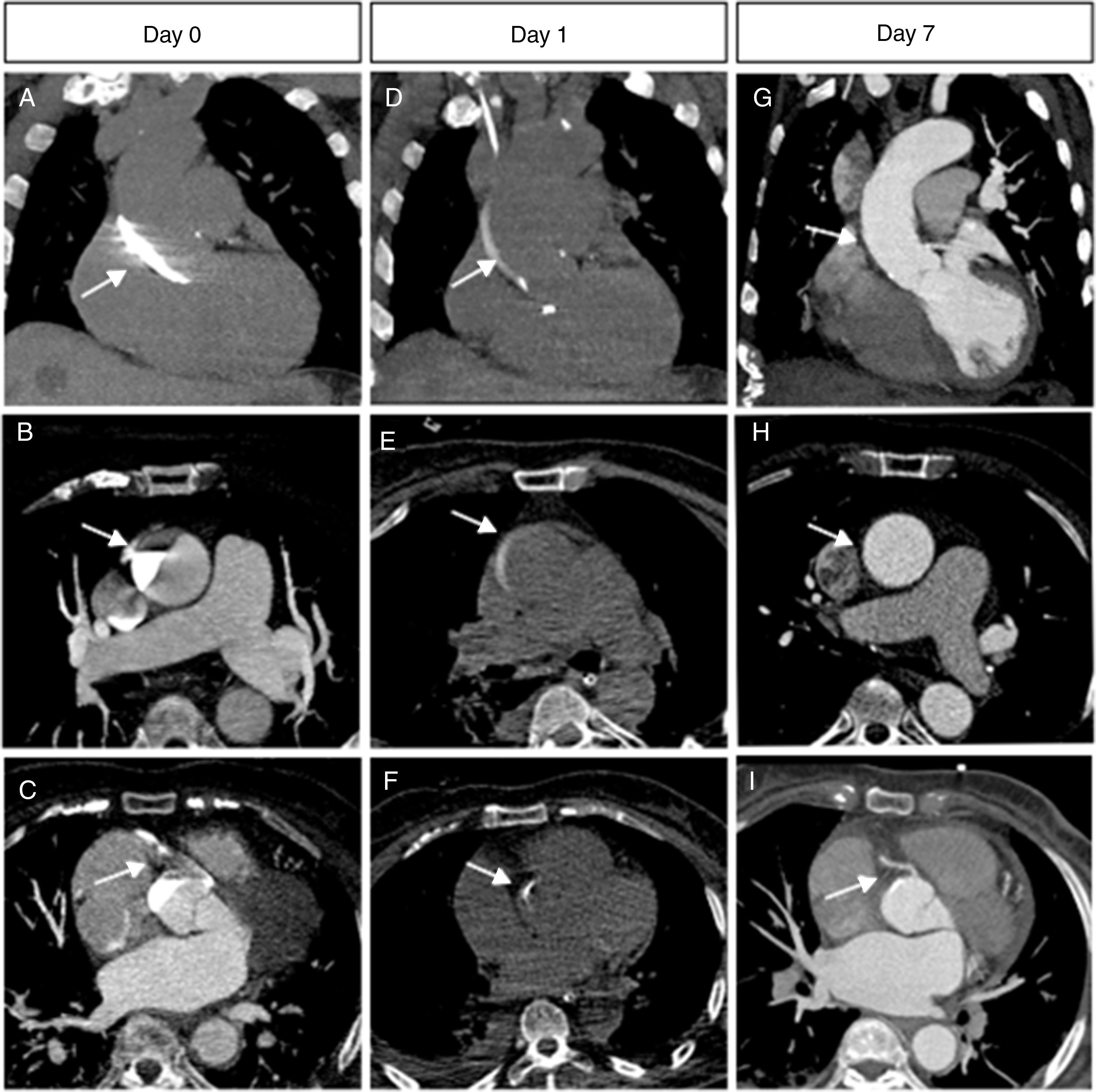
Left CA showed no coronary disease. After the first contrast injection in the right coronary artery (RCA)—which also excluded disease—a radiopaque area was seen in the aortic wall, suggesting catheter-induced (iatrogenic) ascending aortic dissection (IAD) (Figure 1, Panel A, arrow). A few minutes later, occlusion of RCA occurred as a result of dissection progression (Figure 1, Panel B, arrow). CT angiography (CTA) performed immediately in the hemodynamics laboratory (same room, moving gantry) confirmed IAD dissection and acute occlusion of the RCA (Figure 2A, B and C, arrows). Angioplasty of RCA was tried without success because it was not possible to catheterize the true lumen. Bedside echocardiogram showed mild depression of global systolic function of the left ventricle with akinesia of the inferior wall and hypokinesia of the free wall of the right ventricle. As percutaneous intervention was not possible, the patient was referred for coronary artery bypass grafting, but this was refused because of the “location” of the infarction, the relative hemodynamic stability of the patient and the lack of signs of dissection progression. A conservative approach was therefore adopted. The patient developed an inferior myocardial infarction but had a good clinical and hemodynamic recovery. Peak troponin I was 11 ng/mL. One week later, repeat CTA revealed IAD regression (Figure 2G and H, arrows) and spontaneous RCA reperfusion (Figure 2I, arrow).
Thin (3 mm) maximal intensity projection reconstructions in coronal (first row) and transverse planes (second and third rows) of the multidetector chest CT scan performed on the first day (Panels A, B, C), on the second day (panels D, E, F) and one week later (Panels G, H, I), showing how the ascending aortic dissection and RCA occlusion and reperfusion evolved.
The authors have no conflicts of interest to declare.