Liver transplantation from living donors is a legal procedure in Turkey. The patient's spouse and relatives within the fourth degree of consanguinity or affinity can be donors. During the surgery, about 40-60% of the donor's liver is removed.
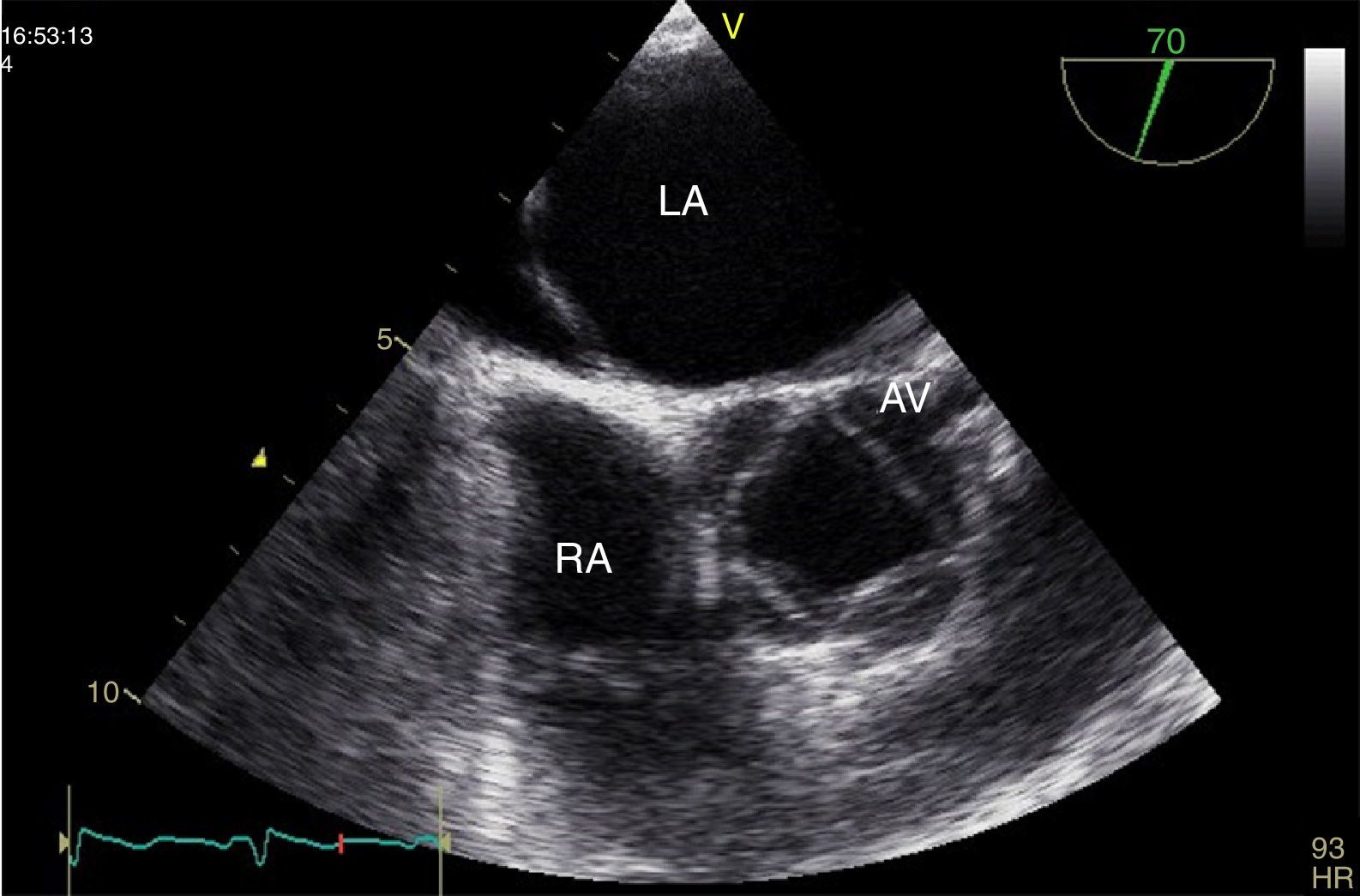
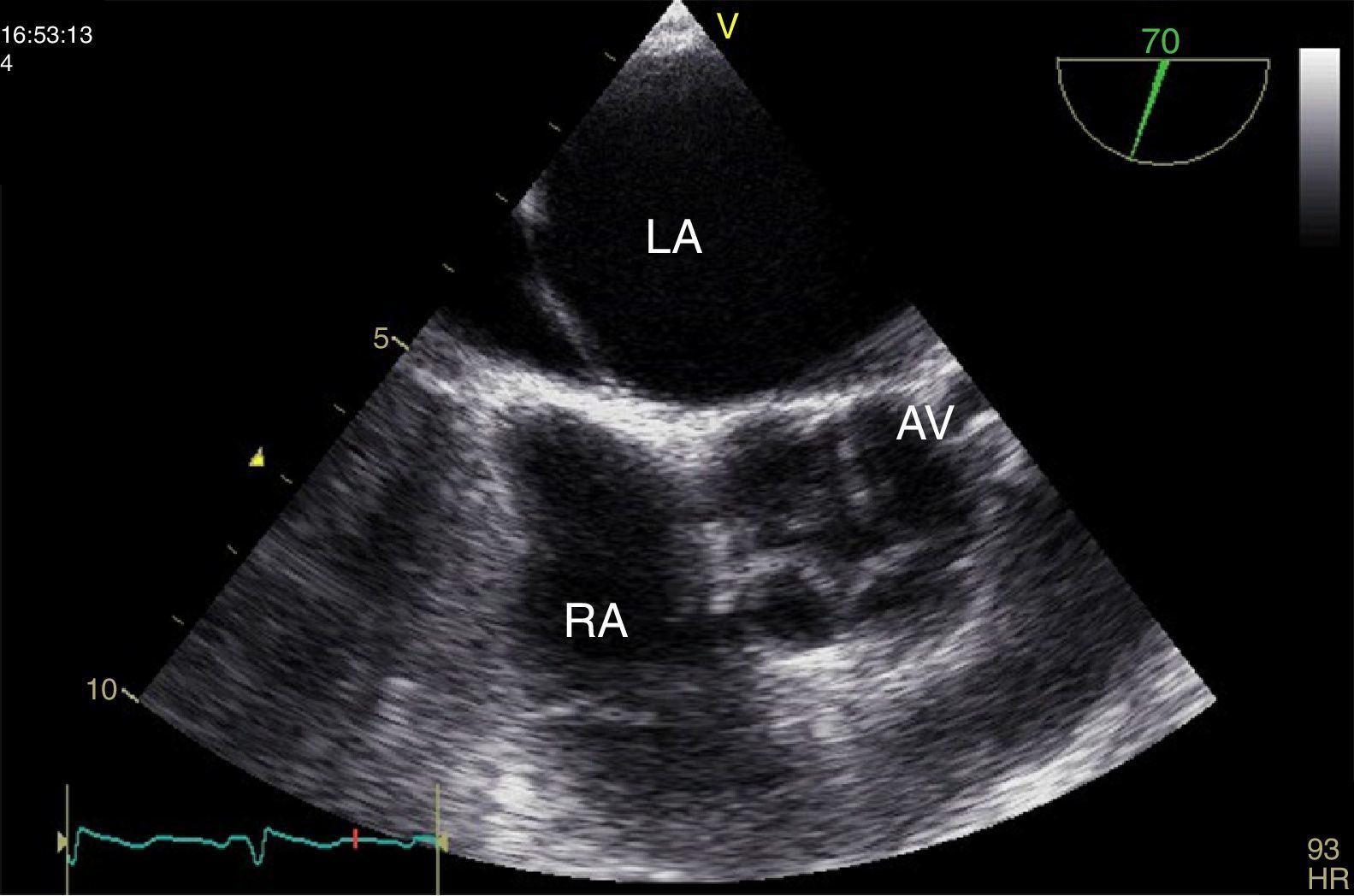
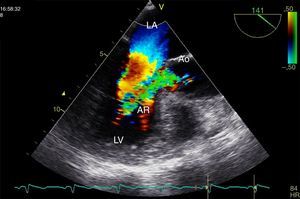
A 38-year-old female liver donor candidate was referred to our cardiology clinic for preoperative evaluation. The patient had no symptoms. On physical examination, a grade 2/6 early diastolic murmur was heard at the third left sternal intercostal space. Her blood pressure was 140/70 mmHg. Transthoracic echocardiography revealed moderate aortic regurgitation (AR) with the suspicion of quadricuspid aortic valve (QAV). Left ventricular end-diastolic and end-systolic diameters were 5.6 cm and 4.0 cm, respectively. Ejection fraction was normal. Transesophageal echocardiography confirmed the diagnosis of QAV with four equal cusps (Type A) (Figures 1 and 2, Video 1) with moderate AR (Figure 3). The patient was removed from the donor list with a suggestion for regular outpatient cardiology clinic visits.
Quadricuspid aortic valve is a rare congenital cardiac anomaly that is mostly diagnosed incidentally. AR usually develops due to fibrosis and incomplete coaptation of the leaflets caused by unequal shear stress. Stenosis can occur but is rare. The risk of infective endocarditis is unknown but there have been documented cases in the literature.
Consequently, if there is unexplained AR, congenital valve anomalies including QAV should be considered as a possible cause.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that no patient data appear in this article.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Conflicts of interestThe authors have no conflicts of interest to declare.