Smoking is associated with atherosclerotic disease, but there is controversy about its protective nature after acute coronary syndrome (ACS).
ObjectiveTo determine the impact of smoking on the presentation, treatment and outcome of ACS.
MethodsWe analyzed all consecutive patients with ACS in a single center between 2005 and 2014. Current smokers and never-smokers were compared. Independent predictors of in-hospital mortality and of a composite of all-cause mortality, rehospitalization for cardiovascular causes, angiography, percutaneous coronary intervention and coronary artery bypass grafting were assessed by multivariate logistic regression.
ResultsA total of 2727 patients were included, 41.7% current smokers and 58.3% never-smokers. Current smokers were younger, more often male, had fewer comorbidities, a typical clinical presentation, lower heart rate, systolic blood pressure, Killip class, BNP/NT-pro-BNP and creatinine, better left ventricular systolic function and less severe coronary anatomy. ST-segment elevation myocardial infarction was more common in current smokers. Current smokers received more evidence-based treatments and had less in-hospital complications, in-hospital mortality and adverse outcomes at one year. More frequent percutaneous coronary intervention at one year was noted in current smokers. Smoking was not an independent predictor of outcome when the multivariate model was fully adjusted for baseline characteristics.
ConclusionThe smoker's paradox was not observed in this population, since all differences in outcome were explained by smokers’ more benign baseline characteristics.
O tabagismo está associado à doença aterosclerótica, mas persistem dúvidas sobre a sua natureza protetora após a ocorrência de uma síndrome coronária aguda.
ObjetivoDeterminar o impacto do tabagismo na apresentação, tratamento e prognóstico das síndromes coronárias agudas.
MetódosAnalisámos todos os doentes consecutivos com síndrome coronária aguda num centro único entre 2005 e 2014. Fumadores activos e não-fumadores foram comparados. Avaliámos os preditores independents de mortalidade intra-hospitalar e de um composto de mortalidade por todas as causas, re-hospitalização de causa cardiovascular, coronariografia, intervenção coronária percutânea e cirurgia de revascularização miocárdica através de regressão logística multivariada.
Resultados2727 dts foram incluídos, 41,7% fumadores e 58,3% não-fumadores. Os fumadores eram mais jovens, mais frequentemente do género masculino, tinham menos comorbilidades, uma apresentação clínica típica e frequência cardíaca, pressão arterial sistólica, classe Killip, BNP/NT-pro-BNP e creatinina mais baixos, função sistólica do ventrículo esquerdo mais alta e doença coronária menos grave. O enfarte agudo do miocárdio com supradesnivelamento do segmento ST foi mais comum nos fumadores. Os fumadores receberam mais frequentmente tratamentos baseados na evidência e tiveram menos complicações e mortalidade intra-hospitalares e eventos adversos no primeiro ano. Uma maior taxa de intervenção coronária percutânea ao primeiro ano foi observada nos fumadores. O tabagismo não foi um preditor independente de prognóstico quando o modelo multivariado foi ajustado para as características basais.
ConclusãoO paradoxo dos fumadores não foi observado nesta população, uma vez que todas as diferenças no prognóstico foram explicadas pelas características basais mais benignas.
acute coronary syndrome
brain natriuretic peptide
coronary artery bypass grafting
confidence interval
disability-adjusted life years
N-terminal pro-brain natriuretic peptide
non-ST-segment elevation myocardial infarction
odds ratio
percutaneous coronary intervention
ST-segment elevation myocardial infarction
upper limit of normal
Tobacco smoking is the leading preventable cause of death worldwide1 and the second leading cause of disability-adjusted life years (DALYs) lost.2 Smoking is strongly associated with the development of atherosclerotic disease, particularly coronary heart disease.2 It is responsible for 10% of all deaths caused by cardiovascular disease and 31% of DALYs lost due to ischemic heart disease.2 However, some studies reported an apparent survival benefit of smokers in the setting of acute coronary syndrome (ACS), ranging from in-hospital mortality3 to three-year mortality,4 a phenomenon known as the ‘smoker's paradox’. Over the years, this concept has been widely disputed and different explanations for this phenomenon have been proposed, based on a biochemical effect or on unmeasured confounding factors.
Firstly, most studies that reported this paradox are from the pre-thrombolytic5,6 and thrombolytic eras,7–13 and smokers are known to have a higher thrombotic burden, which could confer a heightened response to thrombolysis.14–16 Secondly, it has been proposed that smokers also have an enhanced response to clopidogrel therapy.17–22 Thirdly, it has been noted that smokers suffer more out-of-hospital death, thus creating a selection bias when assessing in-hospital mortality.23,24 Lastly, smokers are younger, have fewer risk factors and comorbidities and are more aggressively treated, and this could also contribute to their better prognosis.13,25–27
Despite this evidence, there are still contemporary studies that show smoking to be an independent predictor of outcome.12,28,29
To shed more light on this discrepancy, our study aims to compare the characteristics of patients with ACS according to their smoking status.
MethodsA total of 3298 consecutive ACS patients were admitted to our tertiary cardiology center between 2005 and 2014. Of these, 203 patients who received fibrinolytic therapy were excluded, due to its possible influence on outcome. The remaining patients were stratified according to self-reported smoking status: current smokers (irrespective of quantity), never-smokers and former smokers. The 391 patients included in the latter group were also excluded from the analysis. The population was thus composed of 2727 subjects. Demographic, clinical, laboratory, echocardiographic, angiographic and treatment data were collected. This was a retrospective cohort study, but all data were collected prospectively during the index hospitalization. The clinical outcomes were in-hospital mortality and a composite of all-cause mortality, rehospitalization for cardiovascular causes, angiography, percutaneous coronary intervention (PCI) and coronary artery bypass grafting (CABG) at one year after discharge. Categorical variables were expressed as percentages and continuous variables as medians ± interquartile range. A family history of premature cardiovascular disease was defined as a first-degree family member with a diagnosis of atherosclerotic cardiovascular disease before the age of 55 (for men) or 65 years (for women). There was a change in laboratory availability of N-terminal pro-brain natriuretic peptide (NT-pro-BNP) to brain natriuretic peptide (BNP) in our center during the study period. Therefore, these values are expressed as the number of times above the upper limit of the normal reference range (ULN). Categorical data were analyzed by the chi-square test and continuous data by the Mann-Whitney U test. Logistic regression models were used to assess for independent predictors of the clinical outcomes. Two-sided p-values <0.05 were considered statistically significant.
ResultsOf the 2727 patients, 41.7% (n=1138) were current smokers and 58.3% (n=1589) never-smokers.
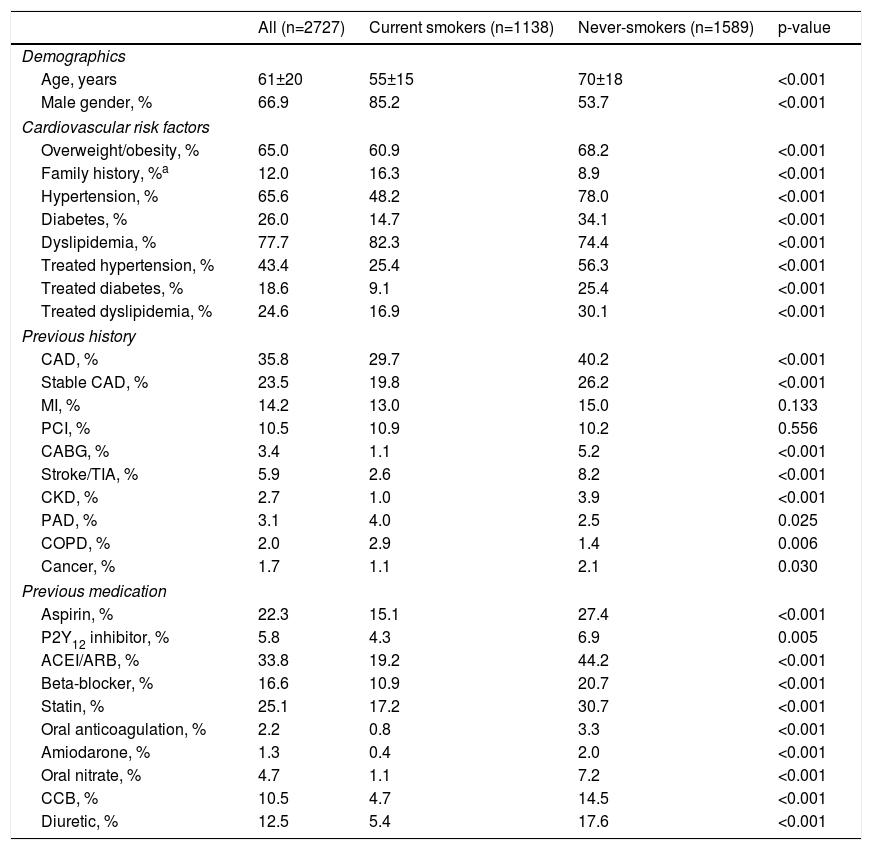
Baseline characteristics differed substantially between current smokers and never-smokers (Table 1). Smokers were significantly younger than never-smokers and more frequently male. They had less classic cardiovascular risk factors, except for dyslipidemia and family history of premature cardiovascular disease, which were more common in smokers. Previous history of coronary artery, cerebrovascular and chronic renal disease were less common in smokers, while chronic obstructive pulmonary and peripheral artery disease were more common, although the overall prevalence was low. Smokers received less treatment for risk factors and had less cardiovascular medication at admission.
Baseline characteristics of patients admitted with acute coronary syndrome according to smoking status.
| All (n=2727) | Current smokers (n=1138) | Never-smokers (n=1589) | p-value | |
|---|---|---|---|---|
| Demographics | ||||
| Age, years | 61±20 | 55±15 | 70±18 | <0.001 |
| Male gender, % | 66.9 | 85.2 | 53.7 | <0.001 |
| Cardiovascular risk factors | ||||
| Overweight/obesity, % | 65.0 | 60.9 | 68.2 | <0.001 |
| Family history, %a | 12.0 | 16.3 | 8.9 | <0.001 |
| Hypertension, % | 65.6 | 48.2 | 78.0 | <0.001 |
| Diabetes, % | 26.0 | 14.7 | 34.1 | <0.001 |
| Dyslipidemia, % | 77.7 | 82.3 | 74.4 | <0.001 |
| Treated hypertension, % | 43.4 | 25.4 | 56.3 | <0.001 |
| Treated diabetes, % | 18.6 | 9.1 | 25.4 | <0.001 |
| Treated dyslipidemia, % | 24.6 | 16.9 | 30.1 | <0.001 |
| Previous history | ||||
| CAD, % | 35.8 | 29.7 | 40.2 | <0.001 |
| Stable CAD, % | 23.5 | 19.8 | 26.2 | <0.001 |
| MI, % | 14.2 | 13.0 | 15.0 | 0.133 |
| PCI, % | 10.5 | 10.9 | 10.2 | 0.556 |
| CABG, % | 3.4 | 1.1 | 5.2 | <0.001 |
| Stroke/TIA, % | 5.9 | 2.6 | 8.2 | <0.001 |
| CKD, % | 2.7 | 1.0 | 3.9 | <0.001 |
| PAD, % | 3.1 | 4.0 | 2.5 | 0.025 |
| COPD, % | 2.0 | 2.9 | 1.4 | 0.006 |
| Cancer, % | 1.7 | 1.1 | 2.1 | 0.030 |
| Previous medication | ||||
| Aspirin, % | 22.3 | 15.1 | 27.4 | <0.001 |
| P2Y12 inhibitor, % | 5.8 | 4.3 | 6.9 | 0.005 |
| ACEI/ARB, % | 33.8 | 19.2 | 44.2 | <0.001 |
| Beta-blocker, % | 16.6 | 10.9 | 20.7 | <0.001 |
| Statin, % | 25.1 | 17.2 | 30.7 | <0.001 |
| Oral anticoagulation, % | 2.2 | 0.8 | 3.3 | <0.001 |
| Amiodarone, % | 1.3 | 0.4 | 2.0 | <0.001 |
| Oral nitrate, % | 4.7 | 1.1 | 7.2 | <0.001 |
| CCB, % | 10.5 | 4.7 | 14.5 | <0.001 |
| Diuretic, % | 12.5 | 5.4 | 17.6 | <0.001 |
Family history of premature cardiovascular disease.
ACEI: angiotensin-converting enzyme inhibitor; ARB: angiotensin receptor blocker; CABG: coronary artery bypass grafting; CAD: coronary artery disease; CCB: calcium channel blocker; CKD: chronic kidney disease; COPD: chronic obstructive pulmonary disease; MI: myocardial infarction; PAD: peripheral artery disease; PCI: percutaneous coronary intervention; TIA: transient ischemic attack.
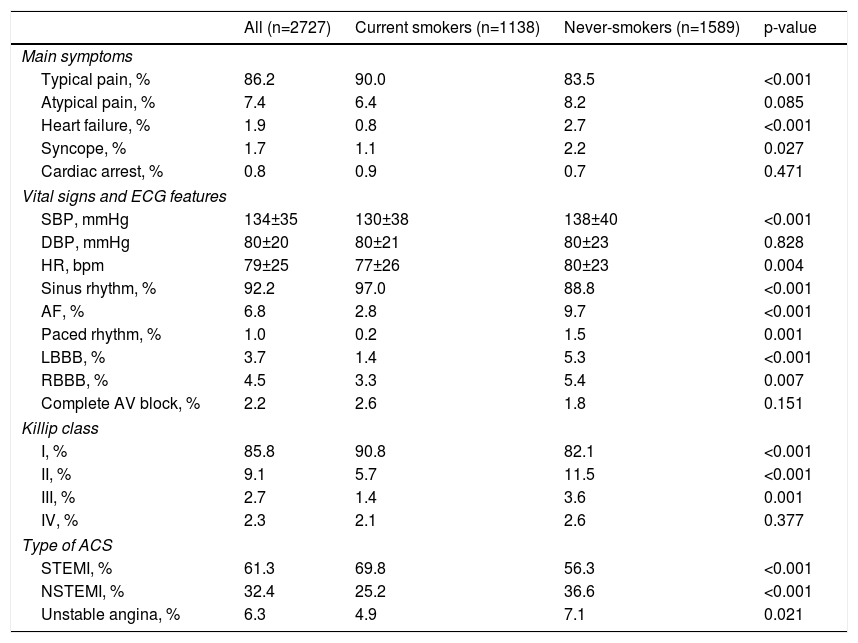
A typical clinical presentation, with lower heart rate, systolic blood pressure and Killip class, and a greater proportion of sinus rhythm at admission were seen among current smokers. ST-elevation myocardial infarction (STEMI) was more common in smokers and non-ST-elevation ACS in non-smokers (Table 2).
Clinical presentation of patients admitted with acute coronary syndrome according to smoking status.
| All (n=2727) | Current smokers (n=1138) | Never-smokers (n=1589) | p-value | |
|---|---|---|---|---|
| Main symptoms | ||||
| Typical pain, % | 86.2 | 90.0 | 83.5 | <0.001 |
| Atypical pain, % | 7.4 | 6.4 | 8.2 | 0.085 |
| Heart failure, % | 1.9 | 0.8 | 2.7 | <0.001 |
| Syncope, % | 1.7 | 1.1 | 2.2 | 0.027 |
| Cardiac arrest, % | 0.8 | 0.9 | 0.7 | 0.471 |
| Vital signs and ECG features | ||||
| SBP, mmHg | 134±35 | 130±38 | 138±40 | <0.001 |
| DBP, mmHg | 80±20 | 80±21 | 80±23 | 0.828 |
| HR, bpm | 79±25 | 77±26 | 80±23 | 0.004 |
| Sinus rhythm, % | 92.2 | 97.0 | 88.8 | <0.001 |
| AF, % | 6.8 | 2.8 | 9.7 | <0.001 |
| Paced rhythm, % | 1.0 | 0.2 | 1.5 | 0.001 |
| LBBB, % | 3.7 | 1.4 | 5.3 | <0.001 |
| RBBB, % | 4.5 | 3.3 | 5.4 | 0.007 |
| Complete AV block, % | 2.2 | 2.6 | 1.8 | 0.151 |
| Killip class | ||||
| I, % | 85.8 | 90.8 | 82.1 | <0.001 |
| II, % | 9.1 | 5.7 | 11.5 | <0.001 |
| III, % | 2.7 | 1.4 | 3.6 | 0.001 |
| IV, % | 2.3 | 2.1 | 2.6 | 0.377 |
| Type of ACS | ||||
| STEMI, % | 61.3 | 69.8 | 56.3 | <0.001 |
| NSTEMI, % | 32.4 | 25.2 | 36.6 | <0.001 |
| Unstable angina, % | 6.3 | 4.9 | 7.1 | 0.021 |
ACS: acute coronary syndrome; AF: atrial fibrillation; AV: atrioventricular; bpm: beats per min; DBP: diastolic blood pressure; ECG: electrocardiographic; HR: heart rate; LBBB: left bundle branch block; RBBB: right bundle branch block; STEMI: ST-segment elevation myocardial infarction; NSTEMI: non-ST-segment elevation myocardial infarction; SBP: systolic blood pressure.
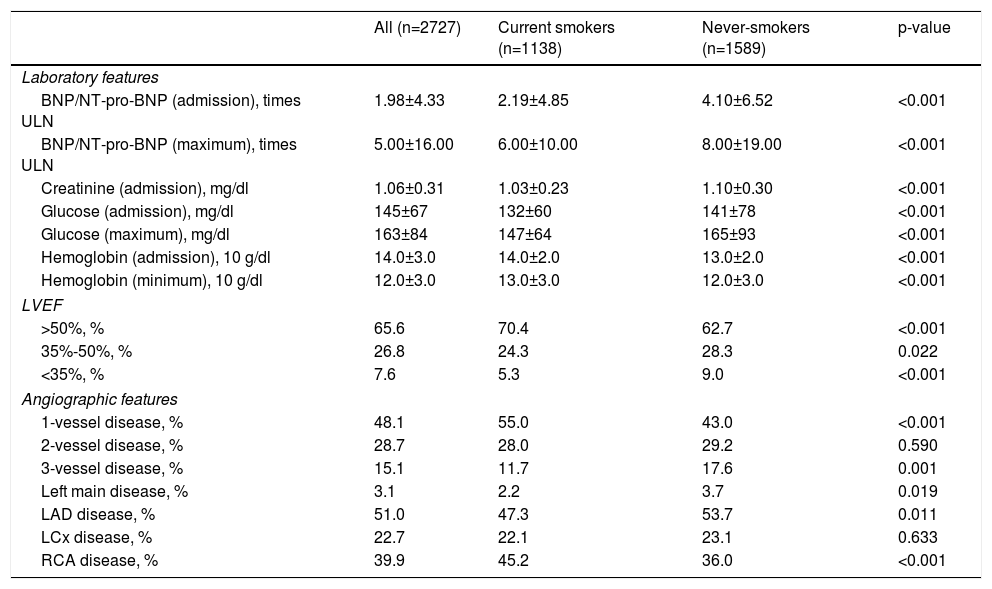
Table 3 displays the laboratory, echocardiographic and angiographic data of the population. Median BNP/NT-pro-BNP, creatinine and glucose values were lower and median hemoglobin levels were higher in smokers compared to never-smokers. Left ventricular systolic dysfunction as assessed by transthoracic echocardiography (left ventricular ejection fraction <50%) was observed less often in smokers, who also had a lower proportion of multivessel, left main and left anterior descending artery disease.
Laboratory, echocardiographic and angiographic data of patients admitted with acute coronary syndrome according to smoking status.
| All (n=2727) | Current smokers (n=1138) | Never-smokers (n=1589) | p-value | |
|---|---|---|---|---|
| Laboratory features | ||||
| BNP/NT-pro-BNP (admission), times ULN | 1.98±4.33 | 2.19±4.85 | 4.10±6.52 | <0.001 |
| BNP/NT-pro-BNP (maximum), times ULN | 5.00±16.00 | 6.00±10.00 | 8.00±19.00 | <0.001 |
| Creatinine (admission), mg/dl | 1.06±0.31 | 1.03±0.23 | 1.10±0.30 | <0.001 |
| Glucose (admission), mg/dl | 145±67 | 132±60 | 141±78 | <0.001 |
| Glucose (maximum), mg/dl | 163±84 | 147±64 | 165±93 | <0.001 |
| Hemoglobin (admission), 10 g/dl | 14.0±3.0 | 14.0±2.0 | 13.0±2.0 | <0.001 |
| Hemoglobin (minimum), 10 g/dl | 12.0±3.0 | 13.0±3.0 | 12.0±3.0 | <0.001 |
| LVEF | ||||
| >50%, % | 65.6 | 70.4 | 62.7 | <0.001 |
| 35%-50%, % | 26.8 | 24.3 | 28.3 | 0.022 |
| <35%, % | 7.6 | 5.3 | 9.0 | <0.001 |
| Angiographic features | ||||
| 1-vessel disease, % | 48.1 | 55.0 | 43.0 | <0.001 |
| 2-vessel disease, % | 28.7 | 28.0 | 29.2 | 0.590 |
| 3-vessel disease, % | 15.1 | 11.7 | 17.6 | 0.001 |
| Left main disease, % | 3.1 | 2.2 | 3.7 | 0.019 |
| LAD disease, % | 51.0 | 47.3 | 53.7 | 0.011 |
| LCx disease, % | 22.7 | 22.1 | 23.1 | 0.633 |
| RCA disease, % | 39.9 | 45.2 | 36.0 | <0.001 |
BNP: brain natriuretic peptide; LAD: left anterior descending artery; LCx: left circumflex artery; LVEF: left ventricular ejection fraction; NT-pro-BNP: N-terminal pro-brain natriuretic peptide; RCA: right coronary artery; times ULN: times above the upper limit of normal.
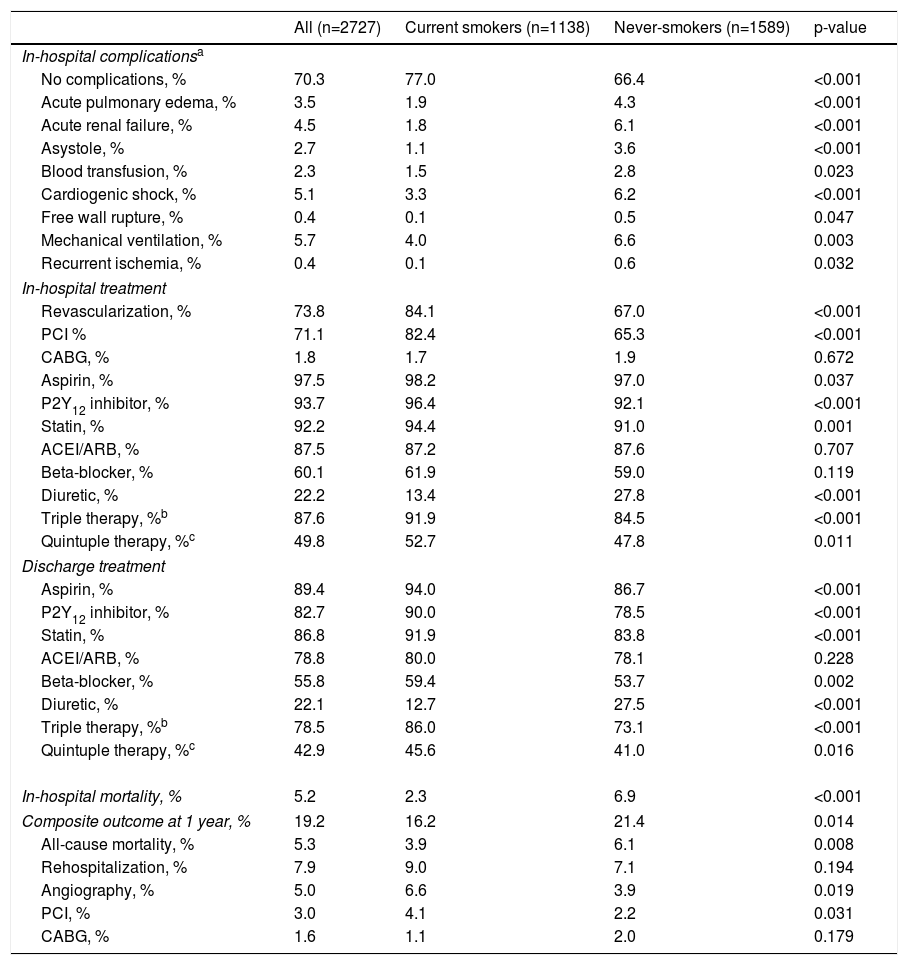
In-hospital complications were least frequent in smokers. They were more often treated by PCI, but there was no difference in CABG. Prescription of aspirin, P2Y12 inhibitors, statin and diuretics during hospital stay and after discharge was significantly lower in never-smokers. Beta-blockers were more widely used in the smokers group at discharge. There was no difference in the use of angiotensin-converting enzyme inhibitors (ACEIs)/angiotensin receptor blockers (ARBs), either in-hospital or at discharge. Smokers were more frequently discharged on a combination of aspirin, P2Y12 inhibitors and statins, and also on a combination of these three drugs plus ACEIs/ARBs and beta-blockers (Table 4).
Complications, treatment and outcome of patients admitted with acute coronary syndrome according to smoking status.
| All (n=2727) | Current smokers (n=1138) | Never-smokers (n=1589) | p-value | |
|---|---|---|---|---|
| In-hospital complicationsa | ||||
| No complications, % | 70.3 | 77.0 | 66.4 | <0.001 |
| Acute pulmonary edema, % | 3.5 | 1.9 | 4.3 | <0.001 |
| Acute renal failure, % | 4.5 | 1.8 | 6.1 | <0.001 |
| Asystole, % | 2.7 | 1.1 | 3.6 | <0.001 |
| Blood transfusion, % | 2.3 | 1.5 | 2.8 | 0.023 |
| Cardiogenic shock, % | 5.1 | 3.3 | 6.2 | <0.001 |
| Free wall rupture, % | 0.4 | 0.1 | 0.5 | 0.047 |
| Mechanical ventilation, % | 5.7 | 4.0 | 6.6 | 0.003 |
| Recurrent ischemia, % | 0.4 | 0.1 | 0.6 | 0.032 |
| In-hospital treatment | ||||
| Revascularization, % | 73.8 | 84.1 | 67.0 | <0.001 |
| PCI % | 71.1 | 82.4 | 65.3 | <0.001 |
| CABG, % | 1.8 | 1.7 | 1.9 | 0.672 |
| Aspirin, % | 97.5 | 98.2 | 97.0 | 0.037 |
| P2Y12 inhibitor, % | 93.7 | 96.4 | 92.1 | <0.001 |
| Statin, % | 92.2 | 94.4 | 91.0 | 0.001 |
| ACEI/ARB, % | 87.5 | 87.2 | 87.6 | 0.707 |
| Beta-blocker, % | 60.1 | 61.9 | 59.0 | 0.119 |
| Diuretic, % | 22.2 | 13.4 | 27.8 | <0.001 |
| Triple therapy, %b | 87.6 | 91.9 | 84.5 | <0.001 |
| Quintuple therapy, %c | 49.8 | 52.7 | 47.8 | 0.011 |
| Discharge treatment | ||||
| Aspirin, % | 89.4 | 94.0 | 86.7 | <0.001 |
| P2Y12 inhibitor, % | 82.7 | 90.0 | 78.5 | <0.001 |
| Statin, % | 86.8 | 91.9 | 83.8 | <0.001 |
| ACEI/ARB, % | 78.8 | 80.0 | 78.1 | 0.228 |
| Beta-blocker, % | 55.8 | 59.4 | 53.7 | 0.002 |
| Diuretic, % | 22.1 | 12.7 | 27.5 | <0.001 |
| Triple therapy, %b | 78.5 | 86.0 | 73.1 | <0.001 |
| Quintuple therapy, %c | 42.9 | 45.6 | 41.0 | 0.016 |
| In-hospital mortality, % | 5.2 | 2.3 | 6.9 | <0.001 |
| Composite outcome at 1 year, % | 19.2 | 16.2 | 21.4 | 0.014 |
| All-cause mortality, % | 5.3 | 3.9 | 6.1 | 0.008 |
| Rehospitalization, % | 7.9 | 9.0 | 7.1 | 0.194 |
| Angiography, % | 5.0 | 6.6 | 3.9 | 0.019 |
| PCI, % | 3.0 | 4.1 | 2.2 | 0.031 |
| CABG, % | 1.6 | 1.1 | 2.0 | 0.179 |
In-hospital complications with non-significant differences between the groups: complete atrioventricular heart block, first or second degree atrioventricular heart block, minor or major bleeding, need for hemodialysis, new bundle branch block, new Q-wave development, reinfarction, severe mitral regurgitation, tamponade, septal rupture, stroke/transient ischemic attack, ventricular fibrillation, ventricular tachycardia.
Combination of aspirin, P2Y12 inhibitor, statin, ACEI/ARB and beta-blocker.
ACEI: angiotensin-converting enzyme inhibitor; ARB: angiotensin receptor blocker; CABG: coronary artery bypass grafting; CAD: coronary artery disease; PCI: percutaneous coronary intervention; STEMI: ST-elevation myocardial infarction.
In-hospital mortality in smokers was a third of that for never-smokers (2.3% vs. 6.9%, p<0.001). The composite outcome of all-cause mortality, rehospitalization for cardiovascular causes, angiography, PCI and CABG at one year was significantly lower in smokers (16.2% vs. 21.4%, p=0.014), driven by lower all-cause mortality (3.6% vs. 6.1%, p=0.008). There was an increased proportion of PCI in smokers at one year (3.9% vs. 2.9%, p=0.029) (Table 4).
When only STEMI was analyzed, the distribution among current and never-smokers of all studied variables was similar to that previously described for the whole spectrum of ACS. There was a tendency for decreased time from symptom onset to first medical contact (90±79 min vs. 106±89 min, p=0.059) and a significantly decreased time from first medical contact to reperfusion (123±113 min vs. 142±131 min, p=0.002) in smokers. Differences in the studied variables were less pronounced for non-ST-segment elevation myocardial infarction (NSTEMI) and unstable angina. In-hospital mortality and the composite endpoint at one year were significantly lower in smokers with STEMI (2.6 vs. 10.1, p<0.001 and 16.2 vs. 21.4, p=0.038, respectively), but there were no differences in patients with NSTEMI or unstable angina.
Smoking was a predictor of in-hospital mortality across the full spectrum of ACS, with an unadjusted odds ratio (OR) of 0.279 (95% confidence interval [CI] 0.181-0.428, p<0.001). However, after adjusting for age, this association was weaker (OR 0.591, 95% CI 0.362-0.965, p=0.036) and when the multivariate model was fully adjusted for all variables with known prognostic significance (age, gender, heart rate, systolic blood pressure, Killip class, creatinine at admission and type of ACS), smoking was not an independent predictor of in-hospital mortality (OR 1.129, 95% CI 0.345-3.696 p=0.842). A similar interaction was seen for STEMI, while for NSTEMI, smoking was not a significant predictor of in-hospital mortality in the univariate analysis. There were no in-hospital deaths in patients with unstable angina. This distribution was reproduced for the composite outcome at one year, and additionally, smoking was also not a predictor in univariate analysis in patients with unstable angina (Table 5).
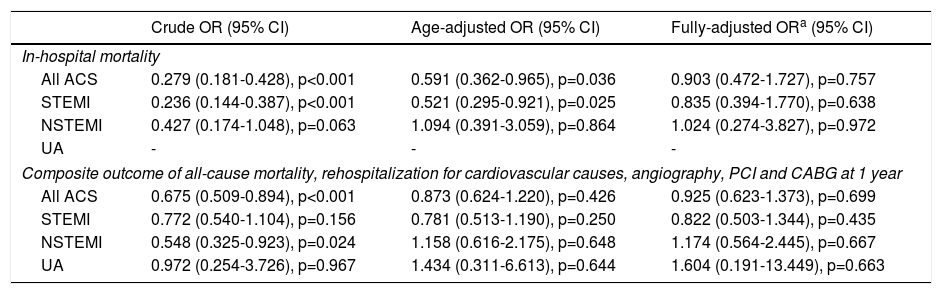
Influence of smoking on in-hospital mortality and on the composite outcome of all-cause mortality, rehospitalization for cardiovascular causes, angiography, PCI and CABG at one year according to type of acute coronary syndrome.
| Crude OR (95% CI) | Age-adjusted OR (95% CI) | Fully-adjusted ORa (95% CI) | |
|---|---|---|---|
| In-hospital mortality | |||
| All ACS | 0.279 (0.181-0.428), p<0.001 | 0.591 (0.362-0.965), p=0.036 | 0.903 (0.472-1.727), p=0.757 |
| STEMI | 0.236 (0.144-0.387), p<0.001 | 0.521 (0.295-0.921), p=0.025 | 0.835 (0.394-1.770), p=0.638 |
| NSTEMI | 0.427 (0.174-1.048), p=0.063 | 1.094 (0.391-3.059), p=0.864 | 1.024 (0.274-3.827), p=0.972 |
| UA | - | - | - |
| Composite outcome of all-cause mortality, rehospitalization for cardiovascular causes, angiography, PCI and CABG at 1 year | |||
| All ACS | 0.675 (0.509-0.894), p<0.001 | 0.873 (0.624-1.220), p=0.426 | 0.925 (0.623-1.373), p=0.699 |
| STEMI | 0.772 (0.540-1.104), p=0.156 | 0.781 (0.513-1.190), p=0.250 | 0.822 (0.503-1.344), p=0.435 |
| NSTEMI | 0.548 (0.325-0.923), p=0.024 | 1.158 (0.616-2.175), p=0.648 | 1.174 (0.564-2.445), p=0.667 |
| UA | 0.972 (0.254-3.726), p=0.967 | 1.434 (0.311-6.613), p=0.644 | 1.604 (0.191-13.449), p=0.663 |
Variables inserted in the model were age, gender, heart rate, systolic blood pressure, Killip class, creatinine at admission and type of ACS (only when considering the full spectrum of ACS).
ACS: acute coronary syndrome; NSTEMI: non-ST-elevation myocardial infarction; STEMI: ST-elevation myocardial infarction; UA: unstable angina.
Our analysis portrays a significant number of patients with ACS admitted to a tertiary cardiology center. We excluded patients who were treated by thrombolysis in view of the need to adjust for the previously described enhanced effect of this therapy in smokers.14–16
The overall prevalence of smoking in this study is similar to those previously published.3,26,30 The decision to exclude former smokers was based on the fact that they are known to have a profile and prognosis intermediate between current smokers and never-smokers, and also include a significant number of patients with previously known coronary artery disease, including myocardial infarction,12,26,31 which could have biased the results.
Smoking is an important determinant of coronary artery disease, as shown by the fact that the smokers’ cohort suffered an ACS on average 15 years before never-smokers, despite having fewer conventional cardiovascular risk factors. The prevalence of dyslipidemia was higher in current smokers, an association that has been described previously.32 Current smokers were also more frequently male, which emphasizes an association with another studied ‘paradox’ in ACS.33–35
The comorbidity profile of smokers is less severe and their presentation is more typical, an observation that could have accounted for patients seeking help more promptly, which is in part suggested by the tendency for lower time from symptom onset to first medical contact (reported only in STEMI). Smoking has been associated with delay in seeking treatment,36 which was not seen in our analysis; this could be related to smokers’ younger age and larger proportion of male subjects.37 Smokers are also more prone to present with ACS as the first manifestation of coronary artery disease, since a history of this entity is less frequent in this group.
Smokers have lower heart rate and systolic blood pressure at admission, as well as lower Killip class and creatinine levels, which are known predictors of better outcome and puts them at an advantage when compared to never-smokers.38
Current smokers have a greater propensity for STEMI.3,26,28,30 Their coronary anatomy is less complex, with less three-vessel disease and fewer left main and left anterior descending lesions, features that are typically associated with a worse prognosis.39
The rate of adherence to evidence-based treatment was greater in smokers, both during the index hospitalization (revascularization and medical treatment)12,26,29–31 and at discharge (medical treatment).31 Moreover, smokers were treated more promptly than never-smokers, as shown by a significantly shorter time from first medical contact to reperfusion (reported only in STEMI).11
In-hospital mortality in smokers was a third of that for never-smokers. Although the composite outcome of all-cause mortality, rehospitalization for cardiovascular causes, angiography, PCI and CABG at one year was lower in smokers, mainly due to lower all-cause mortality, there was a significantly increased rate of repeat PCI in this group. This association has been described in previous reports.40–42
Smoking was associated with in-hospital mortality and adverse outcome at one year, particularly in STEMI, but this association was weaker after adjustment for age and disappeared when other variables with known prognostic impact38 were inserted into the model. Other reports have shown that age may be the sole factor responsible for the smoker's paradox.25,26 This was not the case in our population, in which other variables related to clinical presentation were also important. Smoking had no influence on outcome in patients with NSTEMI and unstable angina, which is in agreement with the initial reports of the smoker's paradox, which referred to STEMI only.9,26,43
This study has some limitations. First, it was retrospective in nature and thus susceptible to inherent limitations. Second, it was not possible to determine the number of pack-years in all smokers. Third, out-of-hospital deaths were not recorded. Fourth, there were no data regarding adherence to medical treatment after discharge.
ConclusionCurrent smokers with ACS were significantly younger and more frequently male, had fewer risk factors and comorbidities, more benign clinical presentation and fewer complications, and received more aggressive treatment. These differences completely explained the lower in-hospital and one-year mortality initially observed in current smokers. Thus, in our population, we did not find a real smoker's paradox. Besides, the apparent benefit was only seen in the subset of patients with STEMI, while differences in overall characteristics were less marked in other types of ACS and no benefit in mortality was seen. Importantly, ACS in smokers occurs around 15 years before never-smokers, which makes smoking a major cardiovascular risk factor and a target for primary and secondary prevention of ischemic heart disease.
Conflicts of interestThe authors have no conflicts of interest to declare.
The authors wish to thank Tiago Pereira da Silva, Pedro Rio, Marta Afonso Nogueira, Andé Viveiros Monteiro, Guilherme Portugal, Pedro Pinto Teixeira, Sílvia Aguiar Rosa, Inês Rodrigues, Luís Almeida Morais and Pedro Modas Daniel for their contributions to the data collection.